BIGBEAR
PHARMACEUTICALS
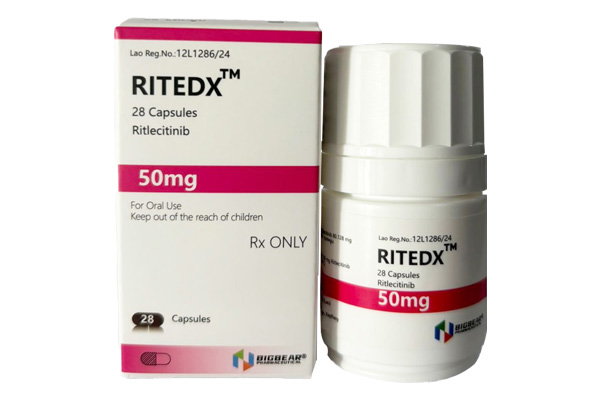
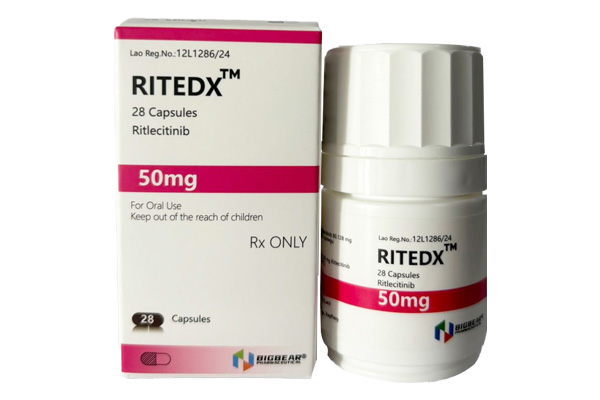
Ritlecitinib is an oral, highly selective inhibitor of JAK3/TEC family kinases and a novel targeted immunomodulatory agent.

 Authentic
Authentic Guarantee
Guarantee Fast Delivery
Fast Delivery Privacy
Privacy Ritlecitinib selectively inhibits the activity of JAK3 and TEC family kinases, precisely blocks abnormal immune signal transduction, and suppresses the pathological attack of the immune system on hair follicles, thereby promoting hair regrowth and improving alopecia symptoms.
Ritlecitinib is a kinase inhibitor indicated for the treatment of severe alopecia areata in adolescents aged 12 years and older and adults.
Combined use with other Janus kinase (JAK) inhibitors, biologic immunomodulators, cyclosporine, or other potent immunosuppressive agents is not recommended.
Prior to initiating treatment with ritlecitinib, the following assessments should be performed:
Tuberculosis (TB) infection assessment:
Initiation of ritlecitinib is not recommended in patients with active TB.
For patients with latent TB or patients who test negative for latent TB but are at high risk of TB, preventive therapy for latent TB should be administered before starting ritlecitinib treatment.
Viral hepatitis screening should be performed in accordance with clinical guidelines.
Initiation of ritlecitinib is not recommended in patients with hepatitis B or hepatitis C.
Treatment should not be initiated in patients with an absolute lymphocyte count (ALC) < 500/mm³ or platelet count < 100,000/mm³.
Vaccination schedules should be adjusted in accordance with current vaccination guidelines.
The recommended dosage of this product is 50mg once daily, taken orally, with or without food.
The capsule should be swallowed whole. Do not crush, split, or chew.
If a dose is missed, it should be taken as soon as possible. However, if the interval is less than 8 hours until the next scheduled dose, the missed dose should not be taken.
Thereafter, continue dosing at the regular scheduled time.
No dosage adjustment is required in patients with mild (Child-Pugh Class A) or moderate (Child-Pugh Class B) hepatic impairment.
Use of ritlecitinib is not recommended in patients with severe (Child-Pugh Class C) hepatic impairment.
Pregnancy
Risk Summary
Data from clinical trials of ritlecitinib use in pregnant women are insufficient to identify a drug‑associated risk of major birth defects, miscarriage, or other adverse maternal or fetal outcomes.
In animal reproduction studies, oral administration of ritlecitinib to pregnant rats and rabbits during organogenesis resulted in fetal toxicity and fetal malformations at exposures approximately 49 and 55 times the maximum recommended human dose (MRHD), respectively.
Lactation
Risk Summary
There are no data on the presence of ritlecitinib in human milk, the effects on the breastfed infant, or the effects on milk production.
Ritlecitinib is excreted in the milk of lactating rats. If a drug is present in animal milk, it is likely that the drug will be present in human milk.
Due to the potential for serious adverse reactions, including serious infections and malignancies, advise women not to breastfeed during treatment with ritlecitinib and for approximately 14 hours (about 6 elimination half‑lives) after the last dose.
The safety and effectiveness of ritlecitinib for the treatment of severe alopecia areata have been established in adolescent patients aged 12 years and older.
The safety and effectiveness of ritlecitinib in pediatric patients below 12 years of age have not been established.
No dosage adjustment is required in patients aged 65 years and older.
A total of 28 subjects aged 65 years and older were enrolled in the alopecia areata trials. Clinical trials of ritlecitinib did not include sufficient numbers of subjects aged 65 years and older, and no subjects aged 75 years and older, to determine whether they respond differently from younger adult patients.
Because the incidence of infections is generally higher in the geriatric population, ritlecitinib should be administered with caution in elderly patients.
Common adverse reactions: Diarrhea.
Less common adverse reactions: Skin blemishes, papules, oral swelling or inflammation.
Ritlecitinib is contraindicated in patients with known hypersensitivity to ritlecitinib or any of its excipients.
Severe infections have been reported in subjects receiving ritlecitinib. The most common severe infections are appendicitis, COVID-19 infection (including pneumonia), and sepsis. Among opportunistic infections, multi-dermatomal herpes zoster has been reported in subjects receiving ritlecitinib.
Avoid use of ritlecitinib in patients with active, severe infections. Before initiating ritlecitinib treatment in patients with the following conditions, the risks and benefits of treatment should be considered:
Patients with chronic or recurrent infections;
Patients with a history of TB exposure;
Patients with a history of severe infections or opportunistic infections;
Patients who have lived or traveled in areas endemic for TB or fungal diseases, or
Patients with underlying conditions that may predispose them to infections.
Patients should be closely monitored for signs and symptoms of infection during and after administration of ritlecitinib. If a patient develops a severe infection or opportunistic infection, ritlecitinib treatment should be interrupted. If a patient develops a new infection during ritlecitinib treatment, timely, comprehensive, and appropriate diagnostic tests suitable for immunocompromised patients should be performed, appropriate anti-infective treatment should be administered, and the patient's condition should be closely monitored. Once the infection is controlled, ritlecitinib treatment may be resumed.
Patients should be screened for tuberculosis (TB) before starting treatment. Ritlecitinib should not be used in patients with active TB. For patients newly diagnosed with latent TB or with previously untreated latent TB, anti-TB treatment should be initiated before starting ritlecitinib treatment. Among patients with negative latent TB screening, anti-TB treatment should be considered first before initiating ritlecitinib treatment in patients with high-risk factors, and screening for TB in high-risk patients during ritlecitinib treatment should be considered.
Viral reactivation, including cases of herpes virus reactivation (e.g., herpes zoster), has been reported in clinical trials. If a patient develops herpes zoster, treatment interruption should be considered until resolution.
Viral hepatitis screening should be performed in accordance with clinical guidelines before initiating ritlecitinib treatment. Patients with evidence of HIV infection or hepatitis B or C infection did not participate in clinical trials.
A large, randomized, post-marketing safety study of another JAK inhibitor in rheumatoid arthritis (RA) patients aged 50 years and older with at least one cardiovascular risk factor showed a higher all-cause mortality rate (including sudden cardiac death) in patients receiving the JAK inhibitor compared with TNF inhibitors. The benefits and risks for individual patients should be considered before initiating or continuing ritlecitinib treatment.
Malignancies, including non-melanoma skin cancer (NMSC), have been observed in clinical trials of ritlecitinib.
A large, randomized, post-marketing safety study of another JAK inhibitor in RA patients showed a higher incidence of malignancies (excluding non-melanoma skin cancer [NMSC]) in patients receiving the JAK inhibitor compared with patients receiving TNF inhibitors. A higher incidence of lymphoma was observed in patients receiving the JAK inhibitor compared with patients receiving TNF inhibitors. A higher incidence of lung cancer was observed in current or past smokers receiving JAK inhibitors compared with those receiving TNF inhibitors. In this study, the risk of all malignancies was additionally increased in current or past smokers.
For patients with a known malignancy (except for cured NMSC or cervical cancer), the risks and benefits of treatment should be considered before initiating or continuing ritlecitinib treatment.
Regular skin examinations are recommended for patients at high risk of skin cancer.
A large, randomized, post-marketing safety study of another JAK inhibitor in RA patients aged 50 years and older with at least one cardiovascular risk factor showed a higher incidence of major adverse cardiovascular events (MACE) in patients receiving JAK inhibitors compared with those receiving TNF inhibitors, where MACE refers to cardiac death, non-fatal myocardial infarction (MI), and non-fatal stroke. The risk was additionally increased in current or past smokers.
The benefits and risks for individual patients should be considered before initiating or continuing ritlecitinib treatment, especially in current or past smokers and patients with other cardiovascular risk factors. Patients should be informed of the symptoms of severe cardiovascular events and their response measures. If a patient experiences a myocardial infarction or stroke, ritlecitinib treatment should be discontinued.
For more detailed drug information, please consult the official package leaflet.
If any issues arise, please contact us immediately.
Email:haiousales@gmail.com

Take ritlecitinib exactly as your healthcare provider tells you to take it. Do not take more or less than prescribed.
Ritlecitinib is taken 1 time a day.
Take with or without food.
Swallow the capsules whole. Do not crush, split, or chew.
Take the missed dose as soon as you remember. Skip the missed dose if it is less than 8 hours before the next dose. Do not use extra medicine to make up for the missed dose.
Temporary treatment interruptions for less than 6 weeks are not expected to result in significant loss of regrown scalp hair.
Avoid receiving a "live" vaccine. Live vaccines include measles, mumps, rubella (MMR), rotavirus, typhoid, yellow fever, varicella (chickenpox), and zoster (shingles).
Tell your doctor about all your other medicines, especially:
CYP3A substrates (such as acetaminophen, codeine, ciclosporin, diazepam, and erythromycin)
CYP3A inducers (such as rifampicin)
CYP1A2 substrates, such as caffeine, clozapine, tacrine, propranolol, and mexiletine.
Should not be used in combination with other JAK inhibitors, biologic immunomodulators, cyclosporine, or other potent immunosuppressants.
This list is not complete. Other drugs may affect ritlecitinib, including prescription and over-the-counter medicines, vitamins, and herbal products. Not all possible drug interactions are listed here.
Copyright2024@ BIGBEAR All right reserved BIGBEAR



