BIGBEAR
PHARMACEUTICAL
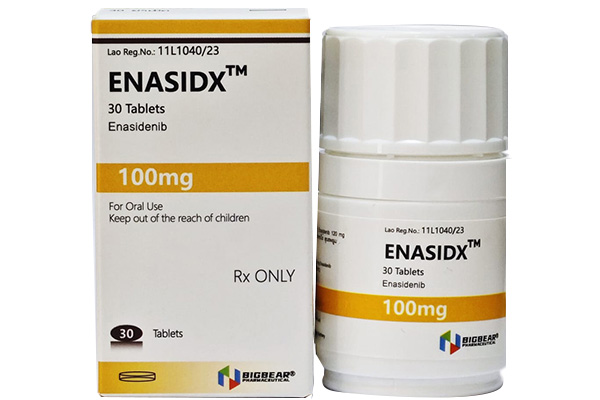
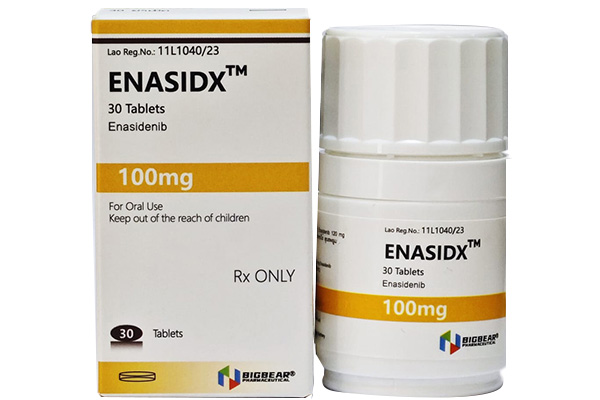
Enasidenib's innovative therapy offers a new treatment option for AML patients who are unresponsive to or experience relapse with conventional therapies.

 Authentic
Authentic Guarantee
Guarantee Fast Delivery
Fast Delivery Privacy
Privacy Enasidenib is an isocitrate dehydrogenase-2 (IDH2) inhibitor that selectively inhibits mutant IDH2 enzyme, reduces the production of the oncogenic metabolite 2-hydroxyglutarate (2-HG), thereby inducing the differentiation of leukemia cells and inhibiting their proliferation.
Enasidenib is indicated for the treatment of adult patients with relapsed or refractory acute myeloid leukemia (AML) who have an isocitrate dehydrogenase-2 (IDH2) mutation detected by an FDA-approved test.
Patients with AML for enasidenib treatment are selected based on the presence of an IDH2 mutation in the blood or bone marrow.
The recommended dose of enasidenib is 100 mg orally once daily, with or without food. Treatment should be continued until disease progression or unacceptable toxicity occurs. For patients without disease progression or unacceptable toxicity, treatment should last for at least 6 months to allow sufficient time for clinical response to develop.
Swallow the tablets whole. Do not chew, split or crush enasidenib tablets. Take enasidenib at approximately the same time each day. If a dose is vomited, missed or not taken at the regular time, take the dose as soon as possible on the same day and resume the normal dosing schedule the next day.
Prior to the initiation of enasidenib treatment, assess blood cell counts and blood chemistry to screen for leukocytosis and tumor lysis syndrome, and monitor at least every 2 weeks for the first 3 months of treatment. Manage any abnormalities promptly. For adverse reactions, treatment interruption or dose reduction is required. The dose adjustment guidelines are as follows:
If differentiation syndrome is suspected, initiate systemic corticosteroid therapy and hemodynamic monitoring. Discontinue enasidenib if severe pulmonary symptoms requiring intubation or ventilator support and/or renal insufficiency persist for more than 48 hours after the start of corticosteroid therapy. Resume enasidenib when signs and symptoms improve to Grade 2 or lower.
Initiate hydroxyurea therapy in accordance with standard institutional practice. If leukocytosis does not improve with hydroxyurea, discontinue enasidenib and resume treatment at a dose of 100 mg once daily when the white blood cell count drops below 30 × 10⁹/L.
Reduce the dose of enasidenib to 50 mg once daily. Resume enasidenib at 100 mg once daily if bilirubin elevation resolves to below 2 × ULN.
Discontinue enasidenib until toxicity resolves to Grade 2 or lower. Resume treatment at 50 mg once daily; the dose may be increased to 100 mg once daily if toxicity resolves to Grade 1 or lower. Permanently discontinue enasidenib if Grade 3 or higher toxicity recurs.
Note: Grade 1 = mild, Grade 2 = moderate, Grade 3 = severe, Grade 4 = life-threatening.
Based on animal embryo-fetal toxicity studies, enasidenib may cause fetal harm when administered to pregnant women. No data are available on the use of enasidenib in pregnant women to assess the risks of drug-related major birth defects and miscarriage. Females are advised to undergo a pregnancy test before taking the drug and consult a physician promptly.
No data are available regarding the presence of enasidenib or its metabolites in human milk, the effects on breastfed infants, or the effects on milk production. Given the potential risk of adverse reactions in breastfed infants, females should be advised not to breastfeed during enasidenib treatment and for 2 months after the last dose.
Based on animal study results, enasidenib may impair fertility in both females and males. It is unknown whether these effects on fertility are reversible.
Advise females of reproductive potential to use effective contraception during enasidenib treatment and for 2 months after the last dose. Coadministration of enasidenib may decrease the concentrations of combined hormonal contraceptives. Advise patients using hormonal contraceptives to use an effective non-hormonal contraceptive method during enasidenib treatment and for 2 months after the last dose.
Advise male partners of females of reproductive potential to use effective contraception during enasidenib treatment and for 2 months after the last dose of enasidenib.
The safety and efficacy of enasidenib in pediatric patients have not been established.
No dose adjustment of enasidenib is required based on age. No overall differences in efficacy or safety were observed between patients aged 65 years or older and younger patients.
Nausea, vomiting, diarrhea, bilirubin elevation and decreased appetite.
Leukocytosis (10%), diarrhea (6%), nausea (5%), vomiting (3%), decreased appetite (3%), tumor lysis syndrome (5%) and differentiation syndrome (8%). Severe differentiation syndrome events include fever, acute renal failure, hypoxia, respiratory failure and multiple organ failure.
Not established.
In clinical trials, 14% of patients receiving enasidenib developed differentiation syndrome, which can be life-threatening or fatal if left untreated. Differentiation syndrome is associated with the rapid proliferation and differentiation of myeloid cells. While there is no diagnostic test for differentiation syndrome, symptoms in patients receiving enasidenib include: acute respiratory distress characterized by dyspnea and/or hypoxia (68%) and the need for supplemental oxygen (76%); pulmonary infiltrates (73%) and pleural effusion (45%); renal impairment (70%); fever (36%); lymphadenopathy (33%); bone pain (27%); peripheral edema with rapid weight gain (21%); and pericardial effusion (18%). Hepatic, renal and multiple organ dysfunction have also been observed.
Differentiation syndrome can occur in patients with or without hyperleukocytosis, as early as 1 day and as late as 5 months after the initiation of enasidenib treatment.
If differentiation syndrome is suspected, initiate oral or intravenous corticosteroid therapy (e.g., dexamethasone 10 mg every 12 hours) and conduct hemodynamic monitoring until the condition improves. Corticosteroid dosage may only be tapered gradually after symptom relief. Premature discontinuation of corticosteroid therapy may lead to a recurrence of differentiation syndrome symptoms. If severe pulmonary symptoms requiring intubation or ventilator support and/or renal insufficiency persist for more than 48 hours after the start of corticosteroid therapy, discontinue enasidenib until signs and symptoms are no longer severe. Hospitalization is recommended for patients with pulmonary and/or renal manifestations for close observation and monitoring.
Based on animal embryo-fetal toxicity studies, enasidenib may cause harm to the embryo and fetus when administered to pregnant women. In animal embryo-fetal toxicity studies, enasidenib induced embryo-fetal toxicity at maternal exposures as low as 0.1 times the steady-state exposure at the recommended human dose (based on area under the concentration-time curve).
Pregnant women should be informed of the potential risks to the fetus. Advise females of reproductive potential to use an effective non-hormonal contraceptive method during enasidenib treatment and for 2 months after the last dose. Advise male partners of females of reproductive potential to use effective contraception during enasidenib treatment and for 2 months after the last dose.
If any issues arise, please contact us immediately.
Email:laosbigbear@gmail.com

Take the missed dose as soon as you remember it on the same day. Resume your once-daily dosing schedule by taking your next dose at your usual time. Do not take two doses within a single day to make up for the missed one.
Seek immediate emergency medical care or contact the Poison Control Center hotline.
Follow your physician’s guidance regarding any restrictions on food, beverages, or physical activity.
Certain medications may interact with enasidenib, including prescription drugs, over-the-counter medications, vitamins, and herbal supplements. Inform your doctor about all medications you are currently taking, as well as any medicines you start or stop using.
Copyright2024@ BIGBEAR All right reserved Bigbear | Bigbear Pharmaceutical | Bigbear Laos



