BIGBEAR
PHARMACEUTICALS
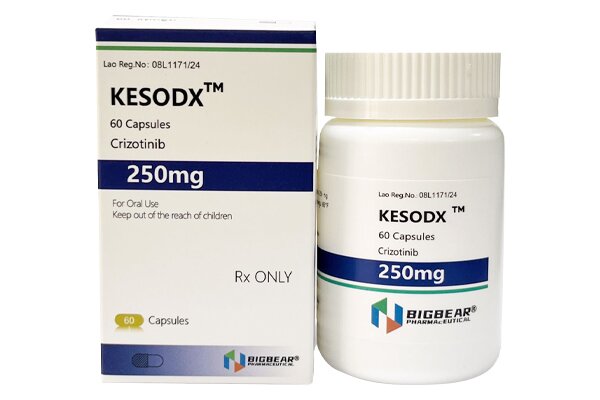
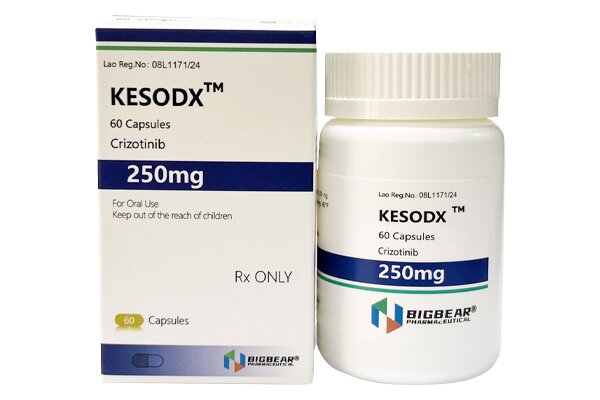
Crizotinib is an oral small-molecule multi-target tyrosine kinase inhibitor, and the world’s first approved targeted antineoplastic agent for both ALK and ROS1. Its common dosage form is capsules.

 Authentic
Authentic Guarantee
Guarantee Fast Delivery
Fast Delivery Privacy
Privacy Crizotinib can selectively inhibit the tyrosine kinase activities of anaplastic lymphoma kinase (ALK), ROS1 and c-MET, block the downstream signal transduction of tumor cells, thereby inhibiting the proliferation and survival of tumor cells.
Crizotinib Capsules are indicated for the treatment of patients with anaplastic lymphoma kinase (ALK)-positive locally advanced or metastatic non-small cell lung cancer (NSCLC).
Crizotinib Capsules are indicated for the treatment of patients with ROS1-positive advanced non-small cell lung cancer (NSCLC).
Crizotinib must be administered in medical institutions with relevant experience and under the guidance of qualified professional personnel.
Prior to initiation of treatment with this product, confirmation of ALK-positive or ROS1-positive status must be obtained using a fully validated test method.
The recommended dosage of Crizotinib Capsules is 250mg orally twice daily, with or without food, until disease progression or unacceptable toxicity occurs.
The capsules should be swallowed whole.
If a dose is missed, the missed dose should be taken unless the next dose is due in less than 6 hours.
If vomiting occurs after administration, the next dose should be taken at the scheduled time.
The recommended dose reduction schedule is as follows:
First dose reduction: 200mg orally twice daily.
Second dose reduction: 250mg orally once daily.
If 250 mg orally once daily is still not tolerated, treatment should be permanently discontinued.
Pregnant Women
Based on animal study results and the mechanism of action of Crizotinib Capsules, administration to pregnant women may cause fetal harm (see [Pharmacology and Toxicology]). No data are available on the use of crizotinib during pregnancy. In animal reproductive studies, oral administration of crizotinib to pregnant rats during organogenesis (at exposures similar to those expected at the maximum recommended human dose) resulted in embryotoxicity and fetotoxicity [see Data]. Pregnant women should be informed of the potential risk of this product to the fetus.
Lactation
No information is available regarding the presence of crizotinib or its metabolites in human milk, or their effects on breastfed infants or milk production. Since adverse reactions may occur in breastfed infants, women are advised not to breastfeed during treatment with crizotinib and for 45 days after the last dose.
Pregnancy Testing
For women of reproductive potential, confirm pregnancy status prior to initiation of Crizotinib Capsules (see [Pharmacokinetics]).
Contraception
Women
Administration of crizotinib to pregnant women may cause fetal harm.
Women of reproductive potential should be advised to use effective contraception during treatment with crizotinib and for at least 45 days after the last dose.
Men
Due to the potential for genotoxicity, men with female partners of reproductive potential should be advised to use condoms during treatment with crizotinib and for at least 90 days after the last dose.
Infertility
Based on results from animal reproductive organ studies, crizotinib may cause impaired fertility in women and men of reproductive potential. It is not known whether the effect on fertility is reversible.
No data on efficacy and safety of Crizotinib Capsules in pediatric patients are available to date.
Among all ALK-positive metastatic non-small cell lung cancer (NSCLC) patients who participated in clinical studies of Crizotinib Capsules (n=1669), 16% were 65 years of age or older, and 3.8% were 75 years of age or older. No overall differences in safety or efficacy were observed between these patients and younger patients.
Clinical studies of Crizotinib Capsules in patients with ROS1-positive metastatic non-small cell lung cancer did not enroll a sufficient number of patients aged 65 years or older to determine whether geriatric patients respond differently to the drug than younger patients.
The most common adverse reactions (≥25%) of Crizotinib Capsules are visual disturbances, nausea, diarrhea, vomiting, edema, constipation, elevated transaminases, fatigue, decreased appetite, upper respiratory tract infection, dizziness and neuropathy.
The most common adverse reactions associated with treatment interruption (≥3%, all-causality frequency) are neutropenia (11%), elevated transaminases (7%), vomiting (5%) and nausea (4%).
The most common adverse reactions associated with dose reduction (≥3%, all-causality frequency) are elevated transaminases (4%) and neutropenia (3%).
Among 302 patients (18%), the most common all-causality adverse reactions associated with permanent treatment discontinuation (≥1%) are interstitial lung disease (1%) and elevated transaminases (1%).
Crizotinib Capsules are contraindicated in patients with hypersensitivity to crizotinib or any ingredient in this product.
When evaluating whether a patient is ALK-positive or ROS1-positive, a fully validated and reliable method must be used to avoid false-negative or false-positive results.
In clinical trials, drug-induced fatal hepatotoxicity occurred in 0.1% of 1719 patients treated with Crizotinib Capsules (see [Adverse Reactions]). Less than 1% of patients treated with Crizotinib Capsules developed elevations in ALT or AST ≥3 times the upper limit of normal (ULN) with concurrent elevations in total bilirubin ≥2 times ULN and normal alkaline phosphatase. Elevations in ALT and AST >5 times ULN occurred in 11% and 6% of patients, respectively. Permanent discontinuation due to elevated transaminases was required in 1.0% of patients. Transaminase elevations typically occurred within the first 2 months of treatment.
Liver function tests, including ALT, AST and total bilirubin, should be performed weekly during the first 2 months of treatment, and monthly thereafter. More frequent repeat testing of transaminases, alkaline phosphatase or total bilirubin should be performed in patients with elevated transaminase levels based on clinical status. Temporary treatment interruption, dose reduction or permanent discontinuation should be implemented according to the instructions in Table 2.
Severe, life-threatening or fatal interstitial lung disease (ILD)/non-infectious pneumonitis may occur in patients treated with Crizotinib Capsules. Based on assessment by the Independent Review Committee (IRC) in patients with ALK-positive non-small cell lung cancer (N=1669), ILD/pneumonitis occurred in 20 patients (1.2%), including 10 patients (<1%) with fatal outcomes. These events typically occurred within the first 3 months of initiation of treatment with Crizotinib Capsules.
In addition, patients should be monitored for pulmonary symptoms if they have indications of ILD/pneumonitis. Treatment with this product should be interrupted if ILD/pneumonitis is suspected. Drug-induced ILD/pneumonitis should be considered in the differential diagnosis of ILD-like disorders (e.g., non-infectious pneumonitis, radiation pneumonitis, hypersensitivity pneumonitis, interstitial pneumonitis, pulmonary fibrosis, acute respiratory distress syndrome [ARDS], alveolitis, pulmonary infiltration, pneumonia, pulmonary edema, chronic obstructive pulmonary disease, pleural effusion, aspiration pneumonia, bronchitis, bronchiolitis obliterans and bronchiectasis). Other potential causes of ILD/non-infectious pneumonitis should be excluded.
Crizotinib treatment should be permanently discontinued in patients who develop treatment-related ILD/non-infectious pneumonitis.
QTc interval prolongation may occur in patients treated with Crizotinib Capsules, which may increase the risk of ventricular tachycardia (e.g., torsades de pointes) or sudden cardiac death. Periodic monitoring of electrocardiogram (ECG), electrolytes and renal function is recommended for patients with congestive heart failure, bradyarrhythmia and electrolyte abnormalities, as well as those receiving antiarrhythmic drugs or other drugs known to prolong the QT interval. Close monitoring of ECG and electrolytes (e.g., serum calcium, magnesium, potassium) should be performed as close as possible to the first dose, and regular monitoring of ECG and electrolytes is recommended, particularly in patients who develop vomiting, diarrhea, dehydration or renal impairment at the start of treatment.
For more detailed drug information, please consult the official package leaflet.
If any issues arise, please contact us immediately.
Email:haiousales@gmail.com

If a dose of crizotinib is missed, it should be taken as soon as you remember. If it is close to the time of the next dose (within 6 hours), the missed dose should be skipped, and the next dose should be taken at the regular time.
If you vomit after taking a dose of crizotinib, do not take an extra dose. The next dose should be taken at the regular time.
Sometimes it is not safe to use certain medications at the same time. Some drugs can affect your blood levels of other drugs you take, which may increase side effects or make the medications less effective. Medications that may interact with crizotinib include:
1.Strong CYP3A inhibitors, such as clarithromycin, erythromycin, diltiazem, itraconazole, ketoconazole, ritonavir, verapamil, goldenseal, and grapefruit. Avoid concomitant use
2.Strong CYP3A inducers, such as phenobarbital, phenytoin, rifampicin, St. John's Wort, and glucocorticoids. Avoid concomitant use
3.CYP3A substrates where minimal concentration changes may lead to serious adverse reactions.
Crizotinib can cause serious heart problems. Your risk may be higher if you also use certain other medicines for infections, asthma, heart problems, high blood pressure, depression, mental illness, cancer, malaria, or HIV.
Not all possible interactions are listed here. Tell your doctor about all your current medicines and any medicine you start or stop using.
Store at room temperature 20° to 25°C (68° to 77°F); excursions permitted between 15° to 30°C (59° to 86°F).
Crizotinib (Xalkori) is an oral kinase inhibitor that may be used to treat:
1.Adults with non-small cell lung cancer which has spread to other parts of the body and is caused by a defect in either a gene called ALK (anaplastic lymphoma kinase) or a gene called ROS1. An ROS1 error occurs in about 1 percent of people with NSCLC, while and ALK error occurs in about 5 percent of cases.
2.Children aged 1 year and older and young adults with anaplastic large cell lymphoma (ALCL) that is ALK-positive. It is used when the ALCL has returned or when a treatment has been tried and it did not work or is no longer working.
3.Adults and children aged 1 year of age and older with ALK-positive inflammatory myofibroblastic tumors (IMT). It is used when the IMT cannot be surgically removed or has returned, or when a treatment has been tried and it did not work or is no longer working.
Crizotinib works by blocking the effects of receptor tyrosine kinases (RTKs), such as ALK, hepatocyte growth factor receptor (HGFR, c-Met), ROS1 (c-ros), and Recepteur d’Origine Nantais (RON). RTKs are essential components of signaling pathways that mediate cell-to-cell communication. Defects in RTKs can result in increased cell proliferation and survival in tumors expressing these proteins. Laboratory research has shown crizotinib-induced cell death and tumor regression in ALCL-derived cell lines that contained nucleophosmin-ALK or c-Met.
Crizotinib was FDA-approved on August 26, 2011. When it was approved, it was the first therapy to be approved for patients with ROS1-positive NSCLC.
Copyright2024@ BIGBEAR All right reserved BIGBEAR



