BIGBEAR
PHARMACEUTICALS
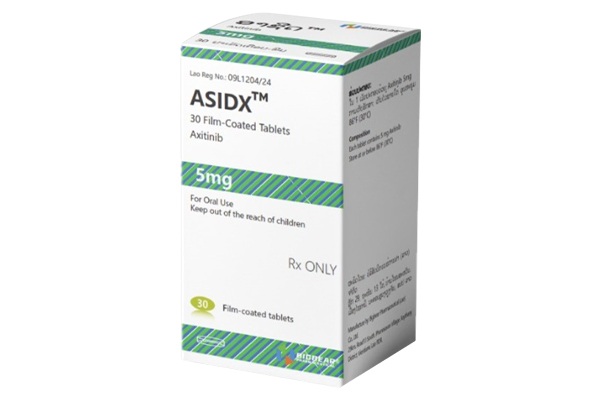
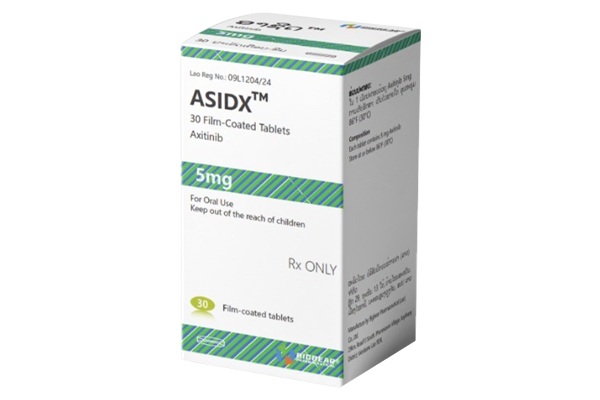
Axitinib is a kinase inhibitor indicated for the treatment of advanced renal cell carcinoma (RCC) following failure of prior systemic therapy.

 Authentic
Authentic Guarantee
Guarantee Fast Delivery
Fast Delivery Privacy
Privacy Apatinib is a targeted anti-cancer drug with apatinib as its main component, which primarily exerts its effect by inhibiting tumor angiogenesis. It can block vascular endothelial growth factor receptors (VEGFR-1, VEGFR-2, and VEGFR-3)—these receptors act as key switches for tumor cells to obtain nutrients, and blocking them can inhibit tumor growth. Clinically, it is mainly used for the treatment of patients with advanced gastric cancer.
This medication is specifically indicated for the treatment of adult patients with advanced renal cell carcinoma (RCC) who have previously received tyrosine kinase inhibitors (a type of targeted drug that blocks cancer cell signal transduction) or cytokine therapy (a biotherapeutic approach that activates the immune system to fight tumors), yet experienced suboptimal therapeutic effects and progressive disease.
1.This medication may be administered to RCC patients presenting with the following conditions: persistent tumor growth and metastasis that cannot be effectively controlled by conventional treatment regimens; cancer cell metastasis to other organs via the blood or lymphatic system; and a physical status that still enables tolerance of targeted drug therapy.
2.It should be noted that this medication can only delay disease progression and is not a curative treatment for cancer. During the medication period, regular imaging examinations (e.g., CT, MRI) are required to monitor changes in tumor size, and physicians will adjust the medication regimen based on the therapeutic response.
1.This medication has a minimal impact on driving ability. However, it should be noted that some patients may experience adverse symptoms such as dizziness and fatigue. The decision to drive should be made prudently based on individual physical reactions.
2.A professional doctor's assessment and guidance are mandatory before medication use; the medication regimen shall not be determined without medical supervision.
1.The treatment is initiated at a dose of 5 mg taken twice daily (with an interval of approximately 12 hours between doses). Continuous administration is required for as long as the treatment is clinically beneficial and well-tolerated by the patient, until severe adverse reactions that cannot be managed or ameliorated by dose adjustment occur.
2.Axitinib tablets should be swallowed whole with warm water. Administration can be with or without food, as food does not affect the drug's efficacy.
Dose escalation may be considered gradually if the patient has received the current dose for more than two consecutive weeks and meets all of the following criteria: no grade 2 or higher adverse reactions (per the internationally accepted adverse reaction grading criteria), maintained normal blood pressure, and no need for antihypertensive medication.
1.First dose escalation: Increase from 5 mg per dose to 7 mg per dose, taken twice daily.
2.Second dose escalation: If the above criteria are still met, the dose may be further increased from 7 mg per dose to 10 mg per dose, taken twice daily.
Dose reduction indications:
1.First dose reduction: Decrease from 5 mg per dose to 3 mg per dose, taken twice daily.
2.Second dose reduction: Decrease from 3 mg per dose to 2 mg per dose, taken twice daily.
1.In case of vomiting or a missed dose, do not take an extra dose to make up for the missed one; take the next scheduled dose as usual.
2.Product information for the same drug manufactured by different pharmaceutical companies may contain discrepancies. If any inconsistency is found, consult a doctor or pharmacist immediately to confirm the appropriate medication regimen.
Special caution is required before and during axitinib treatment. Patients must maintain stable blood pressure and monitor blood pressure values regularly; monitor for elevations in hemoglobin or hematocrit; pay close attention to cardiac function status; and undergo regular thyroid function tests. Any adverse symptoms experienced during treatment must be communicated to a doctor promptly.
This drug is contraindicated in patients with a known hypersensitivity to any of its ingredients.
Administration is contraindicated during pregnancy. If the medication is deemed absolutely necessary, the patient must be informed of the potential risks to the fetus, including the risk of developmental abnormalities and severe malformations.
It is currently unknown whether the drug ingredients are excreted in human breast milk. Since most drugs pass into breast milk and may cause severe adverse reactions in infants, a decision must be made to either discontinue breastfeeding or stop the medication, based on the clinical necessity of treatment.
The safety and efficacy of this drug in pediatric populations have not been established.
Geriatric patients may receive the regular adult dose without dose adjustment.
1.Patients with mild hepatic impairment (Child-Pugh Class A): May receive the regular adult dose without adjustment.
2.Patients with moderate hepatic impairment (Child-Pugh Class B): The initial dose must be reduced by half.
3.Patients with severe hepatic impairment (Child-Pugh Class C): Administration is contraindicated.
Patients with mild to severe renal impairment may receive the regular adult dose. Caution is advised in patients with end-stage renal disease (CLcr < 15 mL/min).
Caution is advised in patients with conditions that may predispose to vascular events, such as hypertension or a history of aneurysm.
Diarrhea, hypertension, fatigue, decreased appetite, nausea, hoarseness, pain and swelling of hands and feet, weight loss, vomiting, generalized weakness, constipation.
Hypothyroidism, cough, mucosal inflammation, arthralgia, oral mucosal ulcer, dyspnea, abdominal pain, headache, limb pain, skin rash, proteinuria, taste disturbance, dry skin, epigastric discomfort, pruritus, alopecia, skin redness.
Dizziness (9%), epigastric pain (8%), myalgia (7%), dehydration (6%), epistaxis (6%), anemia (4%), hemorrhoids (4%), hematuria (3%), tinnitus (3%), elevated blood lipids (3%), tongue pain (3%), pulmonary thromboembolism (2%), rectal hemorrhage (2%), hemoptysis (2%), lower extremity venous thrombosis (1%), retinal vascular occlusion (1%), erythrocytosis (1%), transient cerebral ischemia (1%).
Severe hypertension and hypertensive crisis, arterial or venous thrombosis, abnormal bleeding, heart failure, gastrointestinal perforation or fistula formation, abnormal thyroid function, reversible posterior leukoencephalopathy syndrome (which may present with headache, seizures, etc.), proteinuria, abnormal liver function indicators, liver injury.
Alectinib must be discontinued immediately in the following situations:
Discontinue immediately if symptoms occur, including headache, seizures, confusion, visual disturbances, or other neurological abnormalities, regardless of whether hypertension is present.
If hypertension remains poorly controlled despite antihypertensive therapy and dose adjustment of alectinib, treatment should be suspended. Once blood pressure returns to normal, therapy may be restarted at a lower dose. If a hypertensive crisis occurs, permanent discontinuation is required.
Alectinib is contraindicated in patients with untreated brain metastases or recent gastrointestinal bleeding. If a bleeding event requiring medical intervention occurs, treatment must be suspended.
Cardiac function should be monitored continuously during treatment. If symptoms of heart failure develop, permanent discontinuation may be necessary.
Discontinue alectinib at least 2 days before elective non-urgent surgery. For major surgery, treatment should be withheld for at least 2 weeks, and restarted only after the wound has fully healed.
If moderate or severe proteinuria is detected, dose reduction or treatment suspension is required. If nephrotic syndrome develops, permanent discontinuation is mandatory.
During treatment, regular monitoring of all relevant indicators is essential. Any physical discomfort should be reported to the doctor promptly, who will assess whether to adjust the treatment plan or implement other medical interventions based on the specific situation.
For more detailed drug information, please consult the official package leaflet.
If any issues arise, please contact us immediately.
Email:haiousales@gmail.com

There is currently no authoritative research data that clearly specifies the exact time required for the drug to take effect.
The half-life of the drug in the body (the time required for the drug concentration to decrease by half) ranges from 2.5 to 6.1 hours. However, there is also a lack of authoritative clinical research data on how long the efficacy can be maintained.
If you forget to take the medication on time, there is no need to make up for the missed dose. Continue to take the next dose at the original scheduled time. Do not increase the dosage without authorization.
If an overdose is suspected, the medication should be stopped immediately, continuous medical observation should be performed on the patient, and appropriate supportive treatment measures should be taken according to the specific situation.
Copyright2024@ BIGBEAR All right reserved BIGBEAR



