BIGBEAR
PHARMACEUTICALS
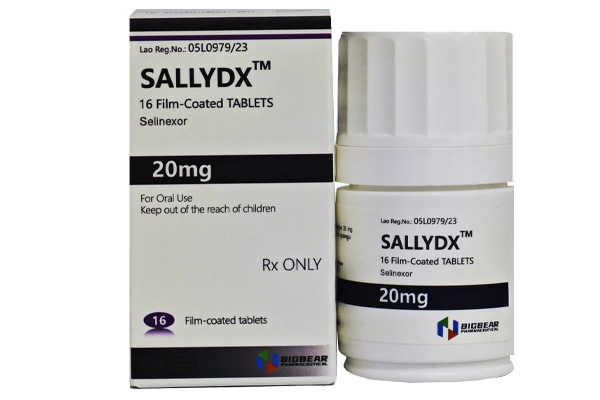
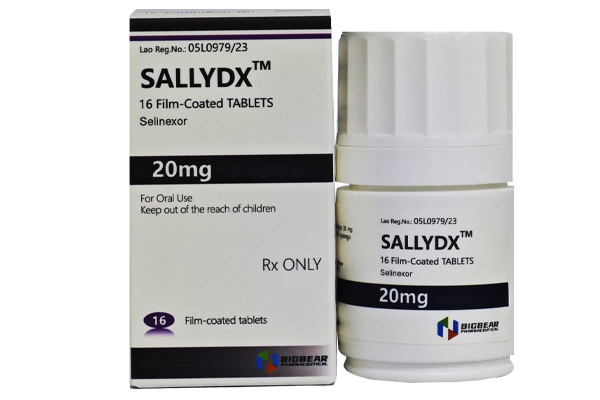
Selinexor has demonstrated significant clinical efficacy in the treatment of relapsed/refractory multiple myeloma and other diseases.

 Authentic
Authentic Guarantee
Guarantee Fast Delivery
Fast Delivery Privacy
Privacy Selinexor acts by binding to the nuclear export protein XPO1 (CRM1), thereby blocking the nuclear export of tumor suppressor proteins, growth regulatory proteins, and anti-apoptotic proteins. This causes these proteins to accumulate in the nucleus and enhances their anti-tumor activity in cells.
This product, in combination with dexamethasone, is indicated for adult patients with relapsed or refractory multiple myeloma who have received prior treatment and are refractory to at least one proteasome inhibitor, one immunomodulatory agent, and one anti-CD38 monoclonal antibody.
This indication is approved conditionally based on the objective response rate and duration of response from a single-arm clinical trial. The efficacy and safety in Chinese patients will be further confirmed post-marketing.
This product as monotherapy is indicated for adult patients with relapsed or refractory diffuse large B-cell lymphoma (DLBCL) who have received at least two prior lines of systemic therapy.
This indication is approved conditionally based on the objective response rate and duration of response from a single-arm clinical trial. Regular approval of this indication will depend on the results of subsequent confirmatory randomized controlled clinical trials.
Selinexor: The recommended dose is 80 mg orally on Days 1 and 3 of each week.
Dexamethasone: The recommended dose is 20 mg orally on Days 1 and 3 of each week, taken together with selinexor.
Selinexor: The recommended dose is 60 mg orally on Days 1 and 3 of each week.
Continue treatment until disease progression or unacceptable toxicity occurs.
Take the tablets at approximately the same time each dosing day, swallowed whole with water. Do not break, chew, crush, or split the tablets.
May be taken with or without food.
If a dose is missed or taken late, take the next dose at the regularly scheduled time.
If vomiting occurs after dosing, do not take an additional dose; take the next dose at the regularly scheduled time.
Monitoring
Before the first dose and during treatment, monitor complete blood counts, standard serum chemistries, body weight, nutritional status, and fluid volume status as clinically indicated. Increase monitoring frequency during the first 3 months of treatment (see [Precautions]). Assess the need for dose adjustments based on adverse reactions.
Hydration and Nutrition
Advise patients to maintain adequate fluid intake and nutrition during treatment. Consider intravenous fluid replacement for patients at risk of dehydration (see [Precautions]).
Antiemetic Prophylaxis
Administer 5-HT3 receptor antagonists and/or other antiemetic medications before the first dose and during treatment (see [Precautions]).
Starting dose: 80 mg orally on Days 1 and 3 of each week (total 160 mg/week).
First reduction: 100 mg/week.
Second reduction: 80 mg/week.
Third reduction: 60 mg/week.
Fourth reduction: Permanent discontinuation.
Starting dose: 60 mg orally on Days 1 and 3 of each week (total 120 mg/week).
First reduction: 40 mg orally on Days 1 and 3 of each week (total 80 mg/week).
Second reduction: 60 mg/week.
Third reduction: 40 mg/week.
Fourth reduction: Permanent discontinuation.
Platelet count 25–75×10⁹/L: Reduce dose by one level and continue treatment.
Platelet count 25–75×10⁹/L with bleeding: Hold treatment; resume at a reduced dose level once bleeding resolves.
Platelet count <25×10⁹/L: Hold treatment; monitor until platelets ≥50×10⁹/L, then resume at a reduced dose level.
Absolute neutrophil count 0.5–1.0×10⁹/L without fever: Reduce dose by one level and continue treatment.
Absolute neutrophil count <0.5×10⁹/L or with fever: Hold treatment; monitor until neutrophils ≥1.0×10⁹/L, then resume at a reduced dose level.
Hemoglobin <8.0 g/dL: Reduce dose by one level and continue treatment; administer blood transfusion or other therapies per clinical guidelines.
Life-threatening anemia: Hold treatment; monitor until hemoglobin ≥8.0 g/dL, then resume at a reduced dose level; administer blood transfusion per clinical guidelines.
Platelet count 50–<75×10⁹/L: Hold one dose; resume at the same dose.
Platelet count 25–<50×10⁹/L without bleeding (first occurrence): Hold treatment; monitor until platelets ≥50×10⁹/L, then resume at the same dose.
Platelet count 25–<50×10⁹/L with bleeding: Hold treatment; monitor until platelets ≥50×10⁹/L, then resume at a reduced dose level once bleeding resolves.
Platelet count <25×10⁹/L: Hold treatment; monitor until platelets ≥50×10⁹/L, then resume at a reduced dose level; administer platelet transfusion per clinical guidelines.
Absolute neutrophil count 0.5–1.0×10⁹/L without fever (first occurrence): Hold treatment; monitor until neutrophils ≥1.0×10⁹/L, then resume at the same dose.
Absolute neutrophil count 0.5–1.0×10⁹/L without fever (recurrence): Hold treatment; monitor until neutrophils ≥1.0×10⁹/L; administer growth factors per clinical guidelines, then resume at a reduced dose level.
Absolute neutrophil count <0.5×10⁹/L or with fever: Hold treatment; monitor until neutrophils ≥1.0×10⁹/L; administer growth factors per clinical guidelines, then resume at a reduced dose level.
Hemoglobin <8.0 g/dL: Resume at a reduced dose level; administer blood transfusion per clinical guidelines.
Life-threatening anemia: Hold treatment; monitor until hemoglobin ≥8.0 g/dL, then resume at a reduced dose level; administer blood transfusion per clinical guidelines.
Grade 1/2 nausea or vomiting (≤5 episodes/day): Maintain dose; add additional antiemetic medications.
Grade 3 nausea or vomiting (≥6 episodes/day or inability to eat/drink): Hold treatment; resume at a reduced dose level once symptoms resolve to ≤Grade 2; add antiemetic medications.
Grade 2 diarrhea (4–6 stools/day, first occurrence): Maintain dose; provide supportive care.
Grade 2 diarrhea (second or subsequent occurrence): Reduce dose by one level; provide supportive care.
Grade 3 or higher diarrhea (≥7 stools/day or hospitalization required): Hold treatment; resume at a reduced dose level once symptoms resolve to ≤Grade 2.
Weight loss 10%–20% or significant malnutrition: Hold treatment; provide supportive care; resume at a reduced dose level once weight recovers to ≥90% of pre-treatment weight.
Serum sodium ≤130 mmol/L: Hold treatment; provide supportive care; monitor until sodium ≥130 mmol/L, then resume at a reduced dose level.
Grade 2 fatigue (≥7 days duration) or Grade 3 fatigue: Hold treatment; resume at a reduced dose level once symptoms resolve to Grade 1 or pre-treatment level.
Grade 2 ocular toxicity (excluding cataracts): Hold treatment; provide supportive care; resume at a reduced dose level once symptoms resolve to Grade 1 or pre-treatment level.
Grade ≥3 ocular toxicity (excluding cataracts): Permanently discontinue treatment; perform ophthalmologic evaluation.
Cataracts (≥Grade 2): Perform ophthalmologic evaluation; resume at a reduced dose level; hold treatment for 24 hours before and 72 hours after cataract surgery.
Hold treatment; resume at a reduced dose level once symptoms resolve to ≤Grade 2.
Females of reproductive potential should avoid pregnancy or sexual intercourse during treatment with this product and for at least 1 week after the last dose. A pregnancy test is recommended before starting treatment. Both females and males of reproductive potential should use effective contraception or avoid sexual intercourse during treatment and for at least 1 week after the last dose to prevent pregnancy.
The pregnancy status of females of reproductive potential must be confirmed before the first dose. There are no clinical data on the use of this product in pregnant women, but animal studies have shown fetal harm.
This product is not recommended for pregnant women or females of reproductive potential who are not using contraception.
If a patient becomes pregnant during treatment, the drug must be discontinued immediately, and the patient should be informed of the potential risks to the fetus.
Based on animal studies, this product may impair fertility in both males and females of reproductive potential.
It is unknown whether this product or its metabolites are excreted in human milk, and the risk to breastfed infants cannot be excluded. Breastfeeding should be discontinued during treatment and for 1 week after the last dose.
The safety and efficacy of this product in patients under 18 years of age have not been established.
In patients with multiple myeloma receiving this product, 47% were aged 65 years and older, and 11% were aged 75 years and older. Compared to patients younger than 75 years, those aged 75 years and older had higher rates of treatment discontinuation due to adverse reactions (52% vs 25%), serious adverse reactions (74% vs 59%), and fatal adverse reactions (22% vs 8%).
In patients with diffuse large B-cell lymphoma receiving this product, 61% were aged 65 years and older, and 25% were aged 75 years and older. The clinical trial of selinexor in patients with relapsed or refractory DLBCL did not include a sufficient number of patients aged ≥65 years to determine whether efficacy differs from that in younger patients.
No dose adjustment is required for patients with mild, moderate, or severe renal impairment. There are no clinical data on the use of this product in patients with end-stage renal disease or those receiving hemodialysis.
No dose adjustment is required for patients with mild hepatic impairment. There are no clinical data on the use of this product in patients with moderate or severe hepatic impairment.
The safety of this product in combination with dexamethasone was evaluated in 214 patients with multiple myeloma, including 83 patients with penta-refractory disease.
The most common adverse reactions (≥30%) were nausea (75%), thrombocytopenia (75%), fatigue (66%), anemia (60%), decreased appetite (56%), weight loss (49%), diarrhea (49%), vomiting (43%), hyponatremia (40%), neutropenia (36%), and leukopenia (30%).
The most frequent serious adverse reactions (≥3%) were infectious pneumonia (7.5%), sepsis (6.1%), thrombocytopenia (4.7%), acute kidney injury (3.7%), and anemia (3.3%).
The safety of this product as monotherapy was evaluated in 127 patients with diffuse large B-cell lymphoma.
The most common adverse reactions (≥20%) were thrombocytopenia (61.4%), nausea (58.3%), fatigue (47.2%), anemia (42.5%), decreased appetite (37.0%), diarrhea (35.4%), constipation (30.7%), neutropenia (29.9%), weight loss (29.9%), vomiting (29.1%), pyrexia (22.0%), and fatigue (21.3%).
The most frequent serious adverse reactions (≥2%) were pyrexia (7.1%), pneumonia (4.7%), sepsis (4.7%, including septic shock, sepsis, and pneumosepsis), fatigue (3.9%), anemia (3.1%), heart failure (3.1%), febrile neutropenia (3.1%), general physical health deterioration (2.4%), hypotension (2.4%), lower respiratory tract infection (2.4%), neutropenia (2.4%), and urinary tract infection (2.4%).
This product is contraindicated in patients with a known hypersensitivity to the active ingredient or any of the excipients.
For more detailed drug information, please consult the official package leaflet.
If any issues arise, please contact us immediately.
Email:haiousales@gmail.com

Copyright2024@ BIGBEAR All right reserved BIGBEAR



