BIGBEAR
PHARMACEUTICALS
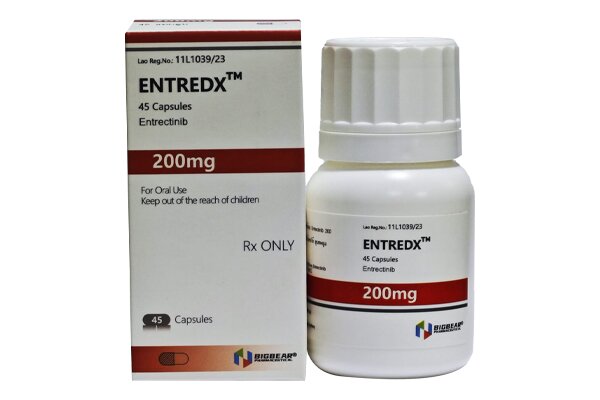
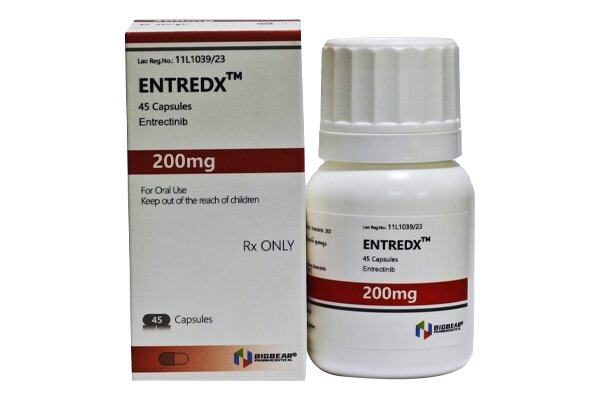
Its unique characteristic is the ability to penetrate the blood-brain barrier, rendering it effective against tumors with central nervous system metastases.

 Authentic
Authentic Guarantee
Guarantee Fast Delivery
Fast Delivery Privacy
Privacy Entrectinib is a tyrosine kinase inhibitor that inhibits the activity of proteins associated with gene fusions involving NTRK1/2/3, ROS1, and ALK, thereby inhibiting tumor cell proliferation.
This product is indicated for adult and pediatric patients aged 1 month and older with solid tumors who meet the following criteria:
Diagnosed with a neurotrophic tyrosine receptor kinase (NTRK) gene fusion (excluding known acquired resistance mutations) via a well-validated detection method;
Have locally advanced, metastatic disease, or disease where surgical resection would likely result in severe complications;
Have no satisfactory alternative treatment options or have failed prior therapies.
This indication was granted conditional approval based on surrogate endpoints. Clinical endpoint data are not yet available, and efficacy and safety will be further confirmed post-marketing.
This product is indicated for adult patients with ROS1-positive locally advanced or metastatic non-small cell lung cancer (NSCLC).
Treatment with this product must be initiated by a physician experienced in anticancer therapy.Prior to treatment, it is mandatory to confirm the presence of an NTRK gene fusion in the patient’s tumor specimen using a validated detection method. Patients whose test results indicate an NTRK gene fusion are eligible for treatment, and the result must be reviewed by an independent third party designated by Roche to confirm the presence of the NTRK gene fusion before treatment can continue.
Patients with locally advanced or metastatic NSCLC must be selected using an empirically validated detection method to confirm ROS1 positivity. ROS1 status must be determined prior to initiating entrectinib treatment.
Capsules: Swallow whole. Do not crush or chew the capsules.
Oral Suspension: For patients who have difficulty swallowing capsules or require enteral administration, an oral suspension prepared from the capsules is available.
The recommended dosage is 600 mg orally once daily, which may be taken with or without food. Do not administer with grapefruit or grapefruit juice. Treatment should continue until disease progression or unacceptable toxicity occurs.
The recommended dosage applies to both adult and pediatric patients, and treatment may be taken with or without food. Do not administer with grapefruit or grapefruit juice. Treatment should continue until disease progression or unacceptable toxicity occurs.
The recommended dosage is 600 mg orally once daily.
Patients with a body surface area (BSA) ≥ 1.51 m²: The recommended dosage is 600 mg orally once daily.
Patients older than 6 months with a BSA of 0.51–0.80 m²: The recommended dosage is 200 mg orally once daily.
Patients older than 6 months with a BSA of 0.81–1.10 m²: The recommended dosage is 300 mg orally once daily.
Patients older than 6 months with a BSA of 1.11–1.50 m²: The recommended dosage is 400 mg orally once daily.
Patients older than 1 month and ≤ 6 months of age: The recommended dosage is 250 mg/m² orally once daily.
Patients ≤ 6 months of age with a BSA ≤ 0.50 m²: The recommended dosage is 300 mg/m² orally once daily.
Note: When dose increments of 10 mg are required, the oral suspension must be prepared from the capsules (see Administration Method).
If a dose is missed, it may be taken as soon as possible unless the next scheduled dose is due within 12 hours. If vomiting occurs immediately after administration, the patient may take another dose.
Swallow the capsules whole. Do not crush or chew them.
Healthcare providers should discuss the volume of water or milk to be added and the volume of suspension to be withdrawn with the patient or caregiver before the first dose (see Table 3 for details).
Instruct the patient or caregiver to carefully open the capsule, empty the contents into room-temperature drinking water or milk, and let it stand for 15 minutes to form the suspension.
Administer the oral suspension immediately after preparation.
If not used within 2 hours (storage temperature ≤ 30°C), discard any unused suspension.
Advise the patient to drink water after taking the oral suspension to ensure complete ingestion of entrectinib.
For patients requiring enteral administration (e.g., via gastrostomy or nasogastric tube), the oral suspension should be administered through the tube. Use an 8 FR or larger enteral tube for volumes of 3 mL or more. Divide doses of 3 mL or more into at least two equal parts and flush the tube with water or milk after each administration. The flushing volume should match the dose volume. For doses of 30 mL, divide into three 10 mL portions and flush the tube with water or milk after each portion. Detailed instructions for preparing and administering the oral suspension via enteral tube are provided in the accompanying package insert.
Starting dose of 250 mg/m² or 300 mg/m²: First reduction to two-thirds of the starting dose; second reduction to one-third of the starting dose. If the patient cannot tolerate after two reductions, permanently discontinue entrectinib.
Starting dose of 200 mg: First reduction to 150 mg once daily; second reduction to 100 mg once daily. If the patient cannot tolerate after two reductions, permanently discontinue entrectinib.
Starting dose of 300 mg: First reduction to 200 mg once daily; second reduction to 100 mg once daily. If the patient cannot tolerate after two reductions, permanently discontinue entrectinib.
Starting dose of 400 mg: First reduction to 300 mg once daily; second reduction to 200 mg once daily. If the patient cannot tolerate after two reductions, permanently discontinue entrectinib.
Starting dose of 600 mg: First reduction to 400 mg once daily; second reduction to 300 mg once daily. If the patient cannot tolerate after two reductions, permanently discontinue entrectinib.
Note: When dose increments of 10 mg are required, the oral suspension must be prepared from the capsules (see Administration Method).
Withhold entrectinib treatment until recovery to Grade ≤ 2 or baseline. Resume treatment at the original or reduced dose based on clinical need.
Withhold entrectinib treatment until recovery to Grade ≤ 1 or baseline. Resume treatment at a reduced dose.
If the adverse event recurs, reduce the dose again.
For persistent, severe, or intolerable events, consider discontinuing treatment based on clinical status.
Grade 3: Withhold entrectinib treatment until recovery to Grade ≤ 1 or baseline. If recovery occurs within 4 weeks, resume treatment at the original dose. If not, permanently discontinue treatment. If a Grade 3 event recurs and recovers within 4 weeks, resume treatment at a reduced dose.
Grade 4: Withhold entrectinib treatment until recovery to Grade ≤ 1 or baseline. If recovery occurs within 4 weeks, resume treatment at a reduced dose. If not, permanently discontinue treatment. If a Grade 4 event recurs, permanently discontinue treatment.
ALT or AST > 3 × ULN and total bilirubin > 2 × ULN (without cholestasis or hemolysis): Permanently discontinue entrectinib treatment.
Initiate urate-lowering therapy.
Withhold entrectinib treatment until signs or symptoms improve. Resume treatment at the original or reduced dose.
Withhold entrectinib treatment until recovery to Grade ≤ 1. Resume treatment at a reduced dose.
Grade 4: Withhold entrectinib treatment until recovery to Grade ≤ 1.
QTc 481–500 ms: Withhold entrectinib treatment until recovery to baseline. Resume treatment at the original dose.
QTc > 500 ms: Withhold entrectinib treatment until the QTc interval recovers to baseline. If the cause of QT prolongation is identified and corrected, resume treatment at the original dose. If other causes are not identified, resume treatment at a reduced dose.
Torsades de pointes, polymorphic ventricular tachycardia, or severe arrhythmia symptoms: Permanently discontinue entrectinib treatment.
Withhold entrectinib treatment until the adverse reaction improves or resolves to Grade 1 or baseline. If recovery occurs within 4 weeks, resume treatment at the original or reduced dose. If not, consider permanently discontinuing treatment. If a Grade 4 event recurs, permanently discontinue treatment.
Avoid concomitant use of strong or moderate CYP3A inhibitors with entrectinib. If unavoidable, reduce the entrectinib dose and limit the duration of concomitant use to 14 days or less.
Starting dose of 200 mg: With a moderate CYP3A inhibitor, reduce to 50 mg once daily; with a strong CYP3A inhibitor, reduce to 50 mg every other day.
Starting dose of 300 mg: With a moderate CYP3A inhibitor, reduce to 100 mg once daily; with a strong CYP3A inhibitor, reduce to 50 mg once daily.
Starting dose of 400 mg: With a moderate CYP3A inhibitor, reduce to 200 mg once daily; with a strong CYP3A inhibitor, reduce to 50 mg once daily.
Starting dose of 600 mg: With a moderate CYP3A inhibitor, reduce to 200 mg once daily; with a strong CYP3A inhibitor, reduce to 100 mg once daily.
After discontinuing the strong or moderate CYP3A inhibitor, resume entrectinib at the dose used before initiation of the inhibitor. A washout period may be required for CYP3A inhibitors with a long half-life.
Note: For pediatric patients with a starting dose < 200 mg, avoid concomitant use of strong or moderate CYP3A inhibitors.
Avoid concomitant use of strong or moderate CYP3A inhibitors with entrectinib.
Avoid concomitant use of CYP3A inducers with entrectinib in adults and pediatric patients.
No studies have been conducted to evaluate the effects of entrectinib on fertility in animals.
Women of reproductive potential must undergo a pregnancy test under medical supervision before initiating entrectinib treatment.
Women of reproductive potential: Must use highly effective contraception during treatment with entrectinib and for 5 weeks after the last dose. Since it is unclear whether entrectinib reduces the efficacy of systemic hormonal contraceptives, women using systemic hormonal contraceptives should be advised to add a barrier method of contraception.
Male patients with female partners of reproductive potential: Must use highly effective contraception during treatment with entrectinib and for 3 months after the last dose, due to the potential genotoxicity of entrectinib.
Women of childbearing potential must be advised to avoid pregnancy during entrectinib treatment (see Warnings and Precautions). There are no data on the use of entrectinib in pregnant women. Based on animal studies (see Pharmacology and Toxicology) and its mechanism of action, entrectinib may cause fetal harm. Patients receiving entrectinib should be informed of the potential risk to the fetus and advised to contact their physician if they become pregnant.
The safety of entrectinib during labor and delivery has not been established.
It is unknown whether entrectinib or its metabolites are excreted in human milk. No studies have been conducted to evaluate the effects of entrectinib on milk production or the presence of entrectinib in milk. Due to the potential risk to breastfeeding infants, mothers are advised to discontinue breastfeeding during entrectinib treatment.
The safety and efficacy of this product have been established in pediatric patients aged 1 month and older. The overall safety profile in pediatric patients aged 1 month and older is generally similar to that observed in adults. However, entrectinib use in pediatric patients is associated with a higher incidence of fractures.
The safety and efficacy of this product in pediatric patients with ROS1-positive locally advanced or metastatic NSCLC have not been established.
No differences in safety or efficacy were observed between patients aged ≥ 65 years and younger patients. No dose adjustment is required for patients aged ≥ 65 years.
No dose adjustment is required for patients with mild or moderate renal impairment. The safety and efficacy of entrectinib in patients with severe renal impairment have not been studied. However, since the renal elimination of entrectinib is negligible, no dose adjustment is needed for patients with severe renal impairment.
The effect of moderate hepatic impairment (total bilirubin > 1.5–3.0 × ULN with normal AST) or severe hepatic impairment (total bilirubin > 3.0 × ULN with normal AST) on the safety of entrectinib at the recommended dose is unknown. Before administering this product to patients with moderate to severe hepatic impairment, the risk-benefit profile of entrectinib should be considered. Patients with hepatic impairment may have an increased risk of adverse reactions, requiring more frequent monitoring for adverse events.
The most common adverse reactions (≥20%) are fatigue, constipation, dysgeusia, edema, dizziness, diarrhea, nausea, hypoesthesia, dyspnea, anemia, weight gain, elevated creatinine, pain, cognitive impairment, vomiting, cough, and pyrexia. Most reported adverse reactions (ADRs) are Grade 1 or 2 in severity.
The most common serious adverse reactions (≥2%) are pulmonary infection (5.2%), dyspnea (4.6%), cognitive impairment (3.8%), pleural effusion (3.0%), and fracture (2.4%).
Permanent discontinuation of treatment due to adverse reactions occurred in 4.6% of patients.
This product is contraindicated in patients with known hypersensitivity to entrectinib or any of its excipients.
The clinical benefit of entrectinib is established based on single-arm studies involving a relatively small population of patients with NTRK fusion-positive solid tumors. In the limited tumor types evaluated, the overall response rate and duration of response demonstrate favorable efficacy. However, efficacy may vary by tumor type and the presence of other concurrent gene mutations (see Pharmacology).
Therefore, entrectinib should only be selected when there are no alternative curative treatment options (e.g., when the clinical benefit of available treatments is unclear or the treatment has already been exhausted).
Cognitive impairment, including confusion, altered mental status, memory impairment, and hallucinations, has been reported in entrectinib clinical trials (see Adverse Reactions for event descriptions). The incidence is higher in patients aged ≥ 65 years than in younger patients. Monitor patients for signs of cognitive changes.
Dose adjustment of entrectinib should be performed according to Table 4 in Dosage and Administration based on the severity of cognitive impairment.
Patients should be informed that entrectinib treatment may cause cognitive changes. Advise patients to avoid driving or operating machinery until symptoms of cognitive impairment resolve (see Ability to Drive and Operate Machinery in Warnings and Precautions).
Entrectinib may increase the risk of fractures (see Specific Adverse Reaction Descriptions in Adverse Reactions). Fractures have occurred in adult and pediatric patients, sometimes following falls, trauma, or disease-related involvement of the affected site, and in some pediatric patients without trauma. There are no data on whether entrectinib affects the healing of existing fractures or the risk of future fractures. Most pediatric patients continued entrectinib treatment and fractures healed.
Promptly evaluate patients for signs or symptoms of fractures (e.g., pain, changes in mobility, deformity).
Hyperuricemia has been observed in patients treated with entrectinib. Assess serum uric acid levels before initiating treatment and periodically during treatment. Monitor patients for signs and symptoms of hyperuricemia. Initiate urate-lowering therapy as clinically indicated and withhold entrectinib if signs or symptoms of hyperuricemia develop.
Dose adjustment of entrectinib should be performed according to Table 4 in Dosage and Administration based on the severity of hyperuricemia.
Cases of congestive heart failure (CHF) have been reported in entrectinib clinical trials (see Table 5 in Adverse Reactions). These events have occurred in patients with and without pre-existing heart disease and resolved with diuretics and/or dose reduction/interruption of entrectinib.
For patients with CHF symptoms or known risk factors, evaluate left ventricular ejection fraction (LVEF) before initiating entrectinib and monitor closely during treatment. Assess patients with clinical signs and symptoms of CHF (including dyspnea or edema) and provide appropriate clinical management.
Dose adjustment of entrectinib should be performed according to Table 4 in Dosage and Administration based on the severity of CHF.
The above information is not exhaustive. For additional details, please refer to the full prescribing information of the medicinal product.
If any issues arise, please contact us immediately.
Email:haiousales@gmail.com

Copyright2024@ BIGBEAR All right reserved BIGBEAR



